Congenital Hypothyroidism: Screening and Management (AAP 2022 Recommendations)
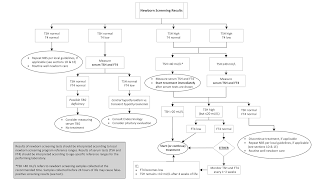
Hypothyroidism Newborn screening (NBS) for CH followed by prompt initiation of levothyroxine (L-T4) therapy can prevent severe intellectual disability, psychomotor dysfunction, and impaired growth. The influence of severity at diagnosis, timing of treatment initiation, and L-T4 dose on longterm outcomes remains a matter of debate. Although the majority of treated patients achieve normal cognitive outcomes, the influence of L-T4 therapy on neurologic development is less certain, and some studies show persistent deficits in treated patients compared with euthyroid healthy controls. If a permanent form of CH has not been established, L-T4 treatment is maintained until 3 years of age, after which thyroid function is reevaluated following a 4- to 6-week discontinuation of L-T4. Most common cause - thyroid dysgenesis, dyshormonogenesis. Less common cause - maternal antithyroid medications, TSH receptor-blocking antibodies (TRBAb) acquired through transplacental passagematernal or infan...